Introducing the WISeR Gold Carding Program

In coordination with CMS, Virtix Health is pleased to announce the upcoming launch of the WISeR Gold Card Exemption Program, set to debut on July 6.
Under the initiative, as outlined on CMS.gov, providers and suppliers who consistently meet coverage criteria by achieving a certain affirmation threshold associated with their prior authorization requests will generally be exempt from any additional prior authorization and pre-payment review processes for the selected items and services in WISeR.
Providers and suppliers who achieve gold card or exemption status will be able to maintain it for a defined period of time before undergoing re-evaluation to ensure they continue to meet Medicare coverage criteria for those selected WISeR services.[1]
To learn more about how the program works and eligibility requirements, see additional details below.
How It Works
Virtix Health will evaluate providers’ and suppliers’ prior authorization requests to determine which providers and suppliers have an affirmation rate above 80% during the evaluation period.
While CMS has indicated that participants may set the threshold as high as 90%, Virtix Health has determined that an 80% threshold for the initial year is more appropriate. Future years’ thresholds may be subject to change but will be communicated to providers and suppliers in advance and will not be adjusted more than once annually. Individual provider/supplier performance will be evaluated across all services and items included in the WISeR program with one composite affirmation score.
Those who achieve this threshold or higher will be notified that they have been added to the exemption list. The first exemption period will begin July 6. Exemption status will be in effect for a period of one year. Virtix Health will retrospectively review up to 10 claims during the 12-month exemption period. Providers and suppliers whose retrospective audit results are not above the established threshold (i.e. 80% during the initial year of WISeR) may lose their gold card status. Virtix Health will communicate any change in gold card status to providers and suppliers at least 60 days in advance of the loss of such status.
Gold card status will be made at the individual provider/supplier level and will apply to all services and items subject to the WISeR program. Virtix will evaluate providers and suppliers on a quarterly basis. Those who achieve exemption status will maintain that status for one year from the effective date of their exemption. Additionally, providers who choose not to participate in the exemption program may opt out by submitting an opt out request to Virtix Health at wiser.support@virtixhealth.com.
Key Dates
- June 1: Virtix Health will communicate provider and supplier exemptions
- July 6: Effective date of initial exemptions
Methodology
Providers and suppliers must have at least 10 prior authorization requests in the measurement period to be evaluated for the gold card program as per WISeR program guidelines.
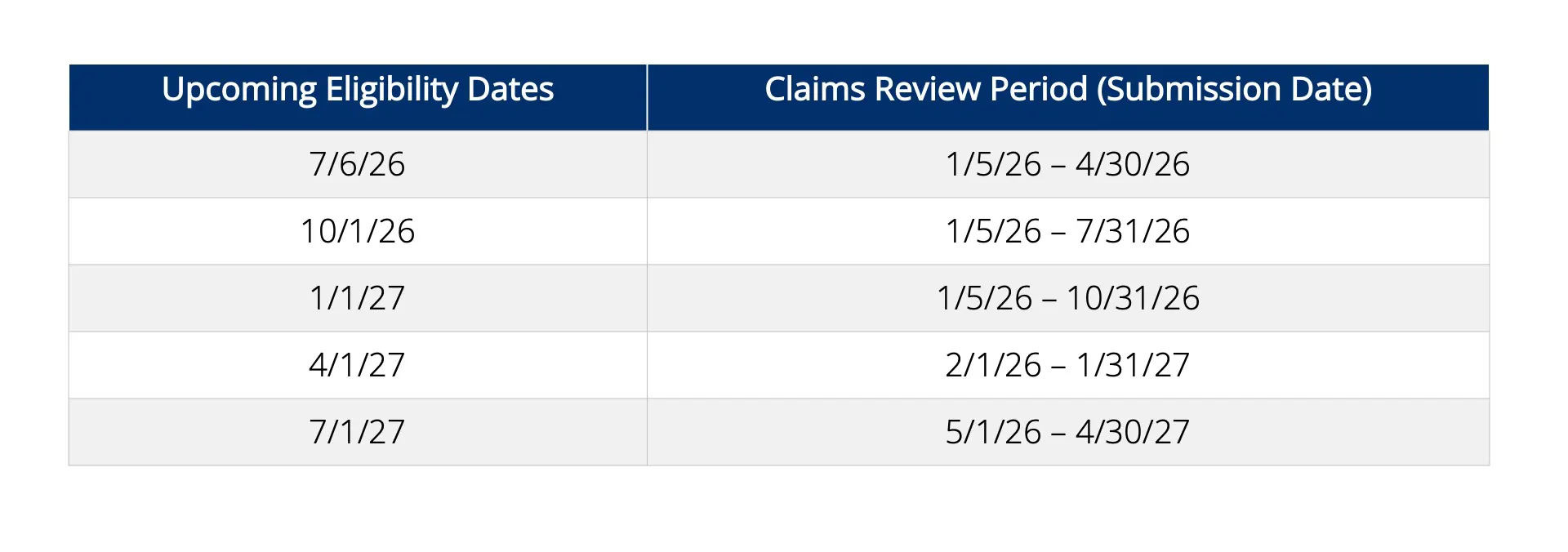
Evaluation period will eventually include up to 12 months of data; however, the first evaluation period will be submissions from January 5 – April 30. The subsequent evaluation periods will include an additional 3 months to this baseline period until it reaches 12 months of data. At which point, it will then become a rolling 12-month evaluation. This will allow for the maximum number of providers and suppliers to be evaluated for the gold card program. Please see table at the end of this fact sheet for report schedule.
Achieving an 80% affirmation rate is evaluated based on the first submission for a prior authorization. Any initial submissions that are dismissed will not be considered a submission.
- Scenario 1: Provider/supplier submits a prior authorization request, and it is initially dismissed. Provider/supplier updates information and resubmits request and it is provisionally affirmed, the submission would be considered affirmed for the gold card evaluation.
- Scenario 2: Provider/supplier submits a prior authorization request and it is initially non-affirmed. Provider/supplier submits additional documentation to achieve an affirmation. The submission would be considered affirmed for the gold card evaluation.
Next Steps
Prior to the finalization of the initial gold card list, Virtix Health will host a webinar with providers and suppliers to answer any questions regarding the program. Providers and suppliers are encouraged to submit their questions to wiser.support@virtixhealth.com. A date and time will be shared in the coming weeks.
[1] https://www.cms.gov/priorities/innovation/files/document/wiser-model-frequently-asked-questions