Provider Portal User Guide
This guide provides step‑by‑step instructions for using the WISeR Provider Portal—from understanding the model and setting up users to submitting requests, managing reviews, and resolving issues.
It equips you with the tools to navigate workflows efficiently, track case status, respond to documentation needs, and access resources that support success in the WISeR program.
The 13 Specific Procedures
Virtix Health’s role is restricted to Washington State and limited to 13 specific procedures that have been pre-determined. These procedures have been identified as high risk for fraud, waste, and abuse. The list of services include:
- Percutaneous Image-Guided Lumbar Decompression for Spinal Stenosis
- Arthroscopic Lavage and Arthroscopic Debridement for the Osteoarthritic Knee
- Induced Lesions of Nerve Tracts
- Vagus Nerve Stimulation
- Phrenic Nerve Stimulator
- Electrical Nerve Stimulators
- Incontinence Control Devices
- Sacral Nerve Stimulation for Urinary Incontinence
- Diagnosis and Treatment of Impotence
- Percutaneous Vertebral Augmentation for Vertebral Compression Fracture
- Epidural Steroid Injections for Pain Management
- Cervical Fusion
- Hypoglossal Nerve Stimulation for the Treatment of Obstructive Sleep Apnea
For WISeR Select Items and Services, Please visit appendix A and C of the CMS WISeR Provider Supplier Guide
How to Access the WISeR Portal
To get started, visit wiser.portal.virtixhealth.com and select Register Now. Registering directly on the provider portal is the preferred and fastest way to receive your login credentials. You will be prompted to provide user information, facility details, and provider information. Once your registration is processed, you will receive a welcome email with your login credentials.
Alternatively, you may request portal access by emailing wiser.support@virtixhealth.com with the subject line “Requesting Portal Access.” Please include your name, email, phone number, facility name and address, facility PTAN, facility NPI, and tax ID. After processing your request, you will receive a welcome email with your login credentials.
1. Welcome to the WISeR Model in the State of Washington
1.1 Welcome
Welcome to the Virtix Health WISeR Program for the State of Washington.
We understand that new programs, especially those involving prior authorization, can feel complex and time-consuming. Our goal with WISeR is to make the process as clear, efficient, and supportive as possible, while protecting access to appropriate, high-quality care for Medicare Beneficiaries.
Virtix Health is here to help you navigate WISeR with confidence.
1.2 What is WISeR?
WISeR (Wasteful and Inappropriate Service Reduction) is a Centers for Medicare & Medicaid Services (CMS) Innovation Model designed to reduce unnecessary, low-value, or potentially harmful services, while supporting timely access to care.
The program focuses on a defined set of outpatient services and uses advanced technology and clinical expertise to ensure requests are reviewed accurately, consistently, and transparently.
1.3 Why WISeR Exists
WISeR was created to address three important goals:
- Protect Medicate Beneficiaries from unnecessary or inappropriate services
- Support physicians with clearer, more consistent review processes
- Reduce administrative burden and rework caused by incomplete or unclear submissions
By aligning submissions more closely with established CMS coverage criteria, WISeR helps streamline decisions and reduce downstream delays.
1.4 How WISeR Supports Patient Care
At its core, WISeR is designed to support the physician-patient relationship.
The program helps to ensure that:
- Requests are reviewed using clear, published CMS guidelines
- Decisions are based on complete, relevant clinical documentation
- Non-affirmed determinations to receive physician review
- Urgent clinical needs can be identified and prioritized
Technology supports the process, but clinical judgement remains central.
1.5 Who is Virtix Health
Virtix Health is the CMS-selected WISeR Participant for the State of Washington.
We support providers and suppliers through:
- A secure, user-friendly submission portal
- AI-enabled technology that assists with CMS eligibility criteria / guideline alignment
- Experienced clinical reviewers, including physicians
- Dedicated support for onboarding, education, and troubleshooting
Importantly, technology does not issue denials. All non-affirmed determinations are reviewed by qualified clinicians.
1.6 Your Relationship with CMS and Noridian
WISeR operates within the existing Medicare framework.
- CMS sets program requirements and coverage policies.
- Noridian remains the Medicare Administrative Contractor (MAC)
- Virtix Health supports the WISeR review workflows with technology and physician expertise
Coverage rules, appeal rights, and payment policies remain unchanged.
1.7 What This Guide Will Help You Do
This guide is designed to help you:
- Understand how WISeR works
- Know when and how to submit requests
- Navigate the Virtix Health WISeR Portal
- Complete submissions accurately and efficiently
- Track cases and respond to the documentation requests
2. Understanding the WISeR Model
Before submitting requests or using the WISeR Portal, it is important to understand how WISeR is structured. WISeR is designed around two distinct review pathways, each with its own purpose and workflow.
2.1 The Two WISeR Pathways
You have two options for WISeR procedures:
- Prior Authorization
- Prior Authorization is a review that occurs before a service is provided.
- This pathway supports appropriate access to care by confirming that requests meet CMS coverage criteria in advance.
OR
- Pre-payment Claim Review
- Prepayment Claim Review is a review that occurs after a service has been provided but before claim payment is issued.
- This pathway focuses on validating documentation related to submitted claims.
These two pathways are distinct and follow different workflows.
2.2 How the WISeR Process Works
WISeR follows the following structure:
- Prior Authorization
- Initial Prior Authorization Request
- Resubmission of a Prior Authorization Request
- Peer-to-Peer (when requested)
OR
- Prepayment Claim Review
- Additional Documentation Request
Each pathway has its own documentation requirements, review steps, and outcomes.
2.3 When to use Expedited Requests
Expedited is a processing priority, not a request type.
Expedited processing may apply to:
- Initial Prior Authorization Requests
- Resubmitted Prior Authorization Requests
Expedited requests must include supporting documentation that delay in performing the procedure could seriously jeopardize the WISeR beneficiary’s life, health, or ability to regain maximum function.
2.4 When to use a Peer-to-Peer
A Peer-to-Peer discussion is a sub-process of Resubmission.
When resubmitting a request, the requester will have the opportunity to request peer-to-peer clinical review to inform the new determination. Under peer-to-peer review, the WISeR provider or WISeR supplier will be connected with a clinician(s) with specialty expertise on the condition under review.
2.5 WISeR Glossary (Canonical Terminology)
This glossary establishes the official terminology used across the Virtix Health WISeR Program, the WISeR Portal, training materials, and support communications.
- Additional Documentation Request (ADR) means a request for additional clinical documentation during Prepayment Claim Review.
- Beneficiary means an individual who is entitled to Medicare FFS benefits under Part A or enrolled under Part B.
- Case Status means the current stage of a Case within the WISeR review process.
- Case means a unique submission record created in the Virtix Health WISeR Portal.
- Digital Intake Form (Cover Sheet) means the digital submission form in the Prior Authorization Management section of the Virtix Health WISeR Provider portal used to create a Case and submit all required information and supporting documentation.
- Enhanced Technology means the WISeR Participant’s technology that is intended to improve the accuracy and efficiency of the Prior Authorization Process and Pre-Payment Review.
- Expedited Processing Priority means the handling of a Case based on urgent medical necessity.
- Expedited means a priority processing request applied to any Prior Authorization or resubmission when a delay in performing the procedure would result in seriously jeopardizing the WISeR beneficiary’s life, health, or ability to regain maximum function.
- Initial Prior Authorization Request means the communication to the WISeR Provider or WISeR Supplier detailing the Prior Authorization Affirmation or Prior Authorization Non-Affirmation for an initial Prior Authorization submission.
- LCDs stands for Local Coverage Determinations and has the meaning set forth in Section 1869(f)(2)(B) of the Social Security Act (42 U.S.C. 1395ff(f)(2)(B)).
- Medical Review means the collection and clinical review of medical records and related information to ensure that Medicare payment is made only for services that meet all Medicare Coverage Criteria.
- Medically Necessary means reasonable and necessary as determined in accordance with Section 1862(a) of the Social Security Act (42 U.S.C. 1395y(a)).
- Medicare Coverage Criteria means the existing Medicare coverage criteria as set forth in statute, regulation, NCD, or LCD.
- Model Participant means a technology company that has signed an agreement with CMS to participate in WISeR and is not the WISeR Participant.
- NCDs stands for National Coverage Determinations and has the meaning set forth in Section 1869(f)(1)(B) of the Social Security Act (42 U.S.C. 1395ff(f)(1)(B).
- Noridian is the Medicare Administrative Contractor (MAC) responsible for claims processing in the State of Washington.
- Peer-to-Peer (P2P) means the clinical discussion requested as part of a Resubmission between the requesting provider and a reviewing physician.
- Pre-payment Claim Review (PPR) means the review by the WISeR Participant to verify consistency with Medicare Coverage Criteria for a claim for one or more Select Items and Services furnished in the MAC Jurisdiction that is submitted to Medicare without requesting Prior Authorization, consistent with 42 C.F.R. § 405.903.
- Prior Authorization (PA) is a request by the WISeR Provider or WISeR Supplier for provisional affirmation of Medicare Coverage Criteria for one of the Select Items and Services prior to furnishing such items and services to the WISeR Beneficiary and before the claim is submitted for processing.
- Prior Authorization Non-Affirmation means a WISeR Provider or WISeR Supplier prior authorization request that is not accepted by the WISeR Participant as meeting the Medicare Coverage Criteria for the Select Item or Service.
- Prior Authorization Provisional Affirmation means a WISeR Provider or WISeR Supplier prior authorization request that is accepted by the WISeR Participant as meeting the Medicare Coverage Criteria for the Select Item or Service.
- Requestor (synonymous with User) means an authorized user who submits and tracks Cases on behalf of a facility. Additionally adds the facility and the provider if they do not already exist in the portal.
- Resubmission means a Prior Authorization submitted to the WISeR Participant within 120 Days of an Initial Prior Authorization Determination for a Prior Authorization previously submitted by the same WISeR Provider or WISeR Supplier for the same WISeR Beneficiary and same Select Item or Service.
- Supporting Documents means the pertinent Clinical records, imaging, test lab results, and other documentation uploaded to support a Case.
- User (synonymous with Requestor) means an authorized user who submits and tracks Cases on behalf of a facility. Additionally adds the facility and the provider if they do not already exist in the portal.
- View Cases means the portal function used to search, filter, and monitor the status of submitted Cases.
- Virtix Health is the CMS-selected WISeR Participant for the State of Washington, providing the WISeR Portal, review workflows, and provider support.
- WISeR (Wasteful and Inappropriate Service Reduction) is the CMS Innovation Model designed to reduce unnecessary, low-value, or potentially harmful outpatient services while supporting timely access to care.
- WISeR Participant means the technology company that meets the requirements set forth in Article III and has signed this Agreement with CMS to participate in the Model.
- WISeR Portal means the secure Virtix Health application used to submit, track, and manage WISeR Cases.
- WISeR Provider means a provider, as that term is defined in 42 C.F.R. § 400.202, that is in the WISeR Participant’s designated WISeR Jurisdiction that furnishes items and services to WISeR Beneficiaries, consistent with Section 3.5.
- WISeR Supplier means a supplier, as that term is defined in 42 C.F.R. § 400.202, that is in the WISeR Participant’s designated WISeR Jurisdiction and who furnishes items and services to WISeR Beneficiaries, consistent with Section 3.5.
3. Getting Started in the Virtix Health WISeR Portal
This section explains who uses the WISeR Portal, how access is managed, and how to sign in.
3.1 WISeR User Roles
Each role has specific responsibilities within the WISeR program.
| Role | What You Do |
| Requestor |
|
| Provider |
|
3.2 How to Request Portal Access
To get started, visit wiser.portal.virtixhealth.com and select Register Now. Registering directly on the provider portal is the preferred and fastest way to receive your login credentials. You will be prompted to provide user information, facility details, and provider information. Once your registration is processed, you will receive a welcome email with your login credentials.
Alternatively, you may request portal access by emailing wiser.support@virtixhealth.com with the subject line “Requesting Portal Access.” Please include your name, email, phone number, facility name and address, facility PTAN, facility NPI, and tax ID. After processing your request, you will receive a welcome email with your login credentials.
3.3 Account Setup & Multi-Factor Authentication
To request access to the Virtix Health WISeR Portal, email: wiser.support@virtixhealth.com
All new users receive an automated welcome email with:
- Username
- Temporary password
- Application URL
- Password requirements
Multi-Factor Authentication (MFA) is required for all users.
Before logging in, download an authenticator app such as:
- Google Authenticator
- Microsoft Authenticator
3.4 Logging in for the first time
Navigate to the application URL provided in your welcome email, then:
- Enter your username and temporary password
- Create a new password
- Set up MFA by scanning the QR code with your authenticator app
- Enter the 6-digit code to complete setup
- For future logins, you will need:
- Your username
- Your password
- Your current authenticator code
4. Requestor/User Setup & Administration
This section explains how Requestor/Users set up facilities, providers, and maintain portal permissions within the Virtix Health WISeR Portal.
4.1 Prior Authorization Management Dashboard Overview
The Prior Authorization Management Dashboard provides a centralized view of:
- Pending Active Requests
- User management tools
Requestor/Users use this dashboard to add facilities and providers, as well as maintain access across their organization.
4.2 Adding Facilities
Requestor/Users are responsible for registering facilities within the WISeR Portal.
To add a facility:
- Log into the Virtix Health WISeR Portal
- Navigate to Prior Authorization Management Dashboard
- Scroll down to Place of Service / Facility Information
- Enter the facility NPI
- Following the pop-up window, select OK to add a new facility
- Enter facility identifying information
- Save the request, then a pop-up window will appear
- Review the facility details
- If correct, agree and confirm to add the facility
- Once confirmed, the facility becomes available for case assignment
Once a Requestor/User has entered the facility NPI, the system will auto-populate details if the facility already exists for future case assignments.
4.3 Adding Providers
Providers are clinicians associated with WISeR cases.
To add a Provider:
- Log into the Virtix Health WISeR Portal
- Navigate to Prior Authorization Management Dashboard
- Scroll down to Attending / Rendering Provider Information
- Enter the provider NPI
- Following the pop-up window, select OK to add a new provider
- Enter provider identifying information
- Save the request, then a pop-up window will appear
- Review the provider details
- If correct, agree and confirm to add the provider
- Once confirmed, the provider becomes available for case assignment
Once a Requestor/User has entered the provider NPI, the system will auto-populate details if the provider already exists for future case assignments.
5. Prior Authorization Workflow
This section explains how to submit Prior Authorization requests in the Virtix Health WISeR Portal. Prior Authorization is a review that occurs before a service is provided and is designed to support timely, appropriate access to care.
5.1 Prior Authorization Overview
Providers may choose to submit Prior Authorization for certain WISeR-applicable services.
Submitting Prior Authorization before care is delivered can help:
- Reduce downstream documentation requests
- Improve timeliness of determinations
- Minimize rework
- Support appropriate patient access
If Prior Authorization is not obtained, documentation may be requested later through Pre-payment Claim Review.
5.2 Initial Prior Authorization Requests
5.2.1 When to Use Initial Requests
Use an Initial Prior Authorization Request when you are submitting an initial request for that beneficiary for that procedure for that date of service.
5.2.2 Step-by-Step Submission
- Log in to the Virtix Health WISeR Portal
- Complete user profile
- Choose Prior Authorization
- Complete user profile
- Select Initial Request
- Complete the Intake Form
- Upload required supporting documentation
- Submit the request
5.2.3 Completing the Intake Form
The Intake Form captures required service, beneficiary, and provider information. All required fields must be completed to avoid processing delays and/or rejection of the request.
5.2.4 Attaching Supporting Documentation
Upload clinical documentation that supports medical necessity, including:
- Office visit notes
- Imaging reports
- Procedure notes
- Relevant lab results
- Any documentation referenced in the coverage guidelines
5.2.5 Submitting & Tracking Status
After submission, the Case status can be monitored under View Cases
5.3 Resubmitting a Prior Authorization Request
5.3.1 When Resubmission is Required
Resubmission is required after an Initial Request is returned or non-affirmed and additional documentation or clarification is submitted.
5.3.2 What Documentation to Include
Include all additional clinical documentation requested in the determination notice.
5.3.3 Step-by-Step Resubmission Process
- Log into the WISeR Portal
- Select the applicable Case
- Choose Resubmission
- Upload additional documentation
- Submit
5.4 Peer-to-Peer Requests (Sub-Workflow)
5.4.1 What Peer-to-Peer Means
Peer-to-Peer is a clinical discussion between the requesting provider and a reviewing physician after a non-affirmation is received by the provider.
5.4.2 When to Request It
Peer-to-Peer may be requested as part of a Resubmission when desired by the treating physician wants to discuss the case with the reviewing physician.
5.4.3 Submitting a Peer-to-Peer Request
- Open the applicable Case
- Select Request Peer-to-Peer
- Provide availability and contact information
- Submit
5.4.4 What Happens Next
A Virtix Health associate will contact the requestor to schedule a time for a reviewing physician to contact the requesting provider to discuss the case.
5.5 Expedited Requests
5.5.1 What Qualifies as Expedited
Expedited requests are used when a delay in care could seriously jeopardize the beneficiary’s life, health, or ability to regain maximum function.
5.5.2 How to Mark a Request as Expedited
Expedited status can be applied to:
- Initial Prior Authorization Requests
- Resubmissions
Select Expedited within the Intake Form and provide supporting documentation.
5.5.3 Documentation Requirements
Supporting documentation must demonstrate a procedure is needed urgently to prevent loss of life, health or the ability to regain maximum function.
1.5.4 Turnaround Time Expectations
When approved for expedited processing, determinations are communicated within two business days of receipt.
6. Pre-payment Claim Review Workflows
This section explains what happens when a claim enters Pre-Payment Claim Review and how to respond to an Additional Documentation Request (ADR). Pre-Payment Claim Review occurs after a service has been provided but before Medicare issue payment.
6.1 Pre-Payment Claim Review Overview
Pre-Payment Claim Review may occur when:
- A claim is submitted for a WISeR-applicable service
- The service has already been delivered
This review protects providers by validating documentation before payment is issued and helps prevent future audits and recoupments.
When your claim enters Pre-Payment Claim Review, you will receive an Additional Documentation Request (ADR).
An ADR will be sent to the Provider, who will have 45-days to return before the medical review may commence. A determination will be issued within 3 days of receiving all necessary documentation.
6.2 Responding to an Additional Documentation Request (ADR)
- Log in to the Virtix Health WISeR Portal
- Navigate to Pre-payment Review Management
- Find your case by including the following information about your claim:
- Claim ID
- Medicare Beneficiary ID
- Procedure Code (any procedure code included in claim may be entered)
6.2.1 Uploading Supporting Documentation
Upload all documentation requested in the ADR within 45 days of the request.
Documentation may include:
- Office visit notes
- Imaging reports
- Lab results
- Procedure notes
- Any other requested clinical documentation
6.2.2 Submitting the ADR Response
After uploading documents:
- Confirm that documentation is complete
- Select Submit
This confirms that your ADR response has been received.
6.2.3 What Happens After Submission
Virtix Health clinical reviewers validate submitted documentation against CMS coverage criteria. Once review is complete:
- The determination is returned to Noridian for claim processing.
7. Tracking & Managing Your WISeR Cases
This section explains how to view, monitor, and manage Cases submitted through the Virtix Health WISeR Portal.
7.1 Viewing Case Status and Determinations
To view your submitted Cases:
- Log into the Virtix Health WISeR Portal
- Select View Cases from the main menu
This screen displays all Cases associated with your account and assigned facilities.
7.2 Understanding Status Messages and Determinations
Each Case displays a status or determination indicating where it is in the review process. Common status messages and determinations include:
| Status | What It Means |
| Submitted | Case has been received |
| In Review | Case is under clinical review |
| Completed-PendingUTN | Review is complete, pending UTN assignment from the MAC |
| ADR Response Pending | Documentation is required for Pre-Payment Claim Review |
| Completed | Review is complete |
| ADR Response Pending | Documentation is required for Pre-Payment Claim Review |
| Completed | Review is complete |
| Determination | What It Means |
| Pending | Case has been received and being validated |
| Dismissed | Case did not meet eligibility criteria for the WISeR Model Program |
| Non-Affirmed | Request did not meet coverage criteria |
| Affirmed | Request meets coverage criteria |
7.3 Searching & Filtering Cases
Use search and filter tools to:
- Locate specific Cases
- Filter by Case Type
- Filter by Status
- Sort by submission date
These tools help manage volume efficiently and keep workflows organized.
8. Troubleshooting & Support
This section provides guidance for common portal issues and how to get help when needed.
8.1 Password Reset
If you forget your password:
- Navigate to the WISeR Portal login page
- Select Forgot Password
- Enter your registered email address
- Follow the password reset instructions sent to your email
8.2 Common Portal Issues
| Issue | What to Do |
| Unable to log in | Confirm your username, password, and MFA code |
| MFA code not accepted | Verify time synchronization on your authenticator app |
| Portal page not loading | Refresh your browser or clear cache |
8.3 Document Upload Issues
File upload criteria:
- Maximum file size: 4 MB
- Maximum number of files per case: 10
- Naming convention: file names must not include any space or special characters
If documents fail to upload:
- Confirm file size and format meet portal requirements
- Try uploading one file at a time
- Verify internet connectivity
- Refresh the browser and retry
8.4 Contacting Support
For WISeR Portal support, contact:
- Email: wiser.support@virtixhealth.com
- Phone: 833-943-2209
Support representatives are available to assist with access, technical issues, and general portal questions Monday – Friday 8am – 4pm EST.
9. Tips for Success in WISeR
The following best practices can help ensure timely, accurate review and reduce delays or additional documentation requests.
9.1 Best Practices for Submissions
- Verify beneficiary eligibility before submitting
- Confirm the service is WISeR-applicable
- Select the correct Case type (Initial, Resubmission, or Pre-Payment Claim Review)
9.2 Documentation Tips
- Include recent and relevant clinical notes
- Attach imaging and lab reports that support medical necessity
- Ensure documentation aligns with CMS coverage guidelines
- Upload legible, complete records
- Avoid submitting duplicate or incomplete files
9.3 Reducing Delays and Denials
- Submit Prior Authorization before care when appropriate
- Respond promptly to ADRs
- Review determination notices carefully
- Maintain accurate portal user access
- Keep facility and provider records current
10. WISeR Resources
This section provides helpful references and support contacts for the WISeR Program.
10.1 CMS WISeR Program Information
For official CMS information about the WISeR Innovation Model, including program updates and coverage policies, visit:
10.2 Noridian Information
Noridian is the Medicare Administrative Contractor (MAC) for the State of Washington. Noridian provides official Medicare claims processing guidance and coverage information. For additional Noridian resources, visit:
10.3 Virtix Health WISeR Support
Virtix Health provides onboarding, training, and portal support for WISeR in the State of Washington.
- Email: wiser.support@virtixhealth.com
- Phone: 833-943-2209
- Portal: wiser.support@virtixhealth.com
10.4 Additional Resources
Additional training materials, FAQs, and portal updates will be provided as the WISeR program evolves.
Quicklinks
Resources

Advancing Appropriate Care Under the WISeR Model
Advancing Appropriate Care Under the WISeR Model Our Role in WISeR: What We Do, How It Works, and Where to Get Help Waste in healthcare can expose patients to unnecessary risk and drive costs without improving outcomes. Estimates suggest that a significant share of...

What to Expect When Your Doctor Requests Prior Authorization
What to Expect When Your Doctor Requests Prior AuthorizationStarting January 5, 2026, Medicare patients in Washington state receiving certain procedures have the option to obtain prior authorization before care is scheduled. This is part of a federal program called...

Introducing the WISeR Gold Carding Program
Introducing the WISeR Gold Carding ProgramIn coordination with CMS, Virtix Health is pleased to announce the upcoming launch of the WISeR Gold Card Exemption Program, set to debut on July 6. Under the initiative, as outlined on CMS.gov, providers and suppliers who...
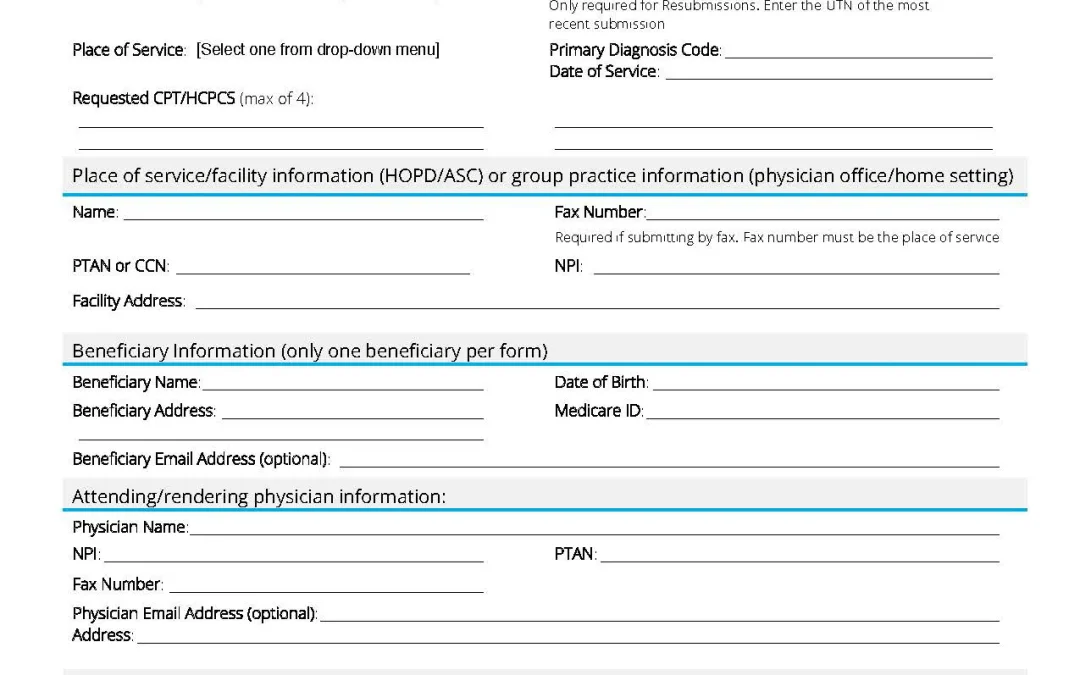
Wiser Manual Intake Form
To save time, web portal submission and electronic document upload will allow you to track the status of your request and receive a quicker response.Manual Non-Portal Submission Download the WISeR intake form for Washington State requests. You may fill this...
